0 Comments
Results published in The British Medical Journal (BMJ) and noted in MedPage Today presented promising evidence that a diet higher in two specific omega-3, fatty acids (EPA and DHA) “reduced headache frequency and intensity and lowered levels of pain-related lipids in migraine patients.”
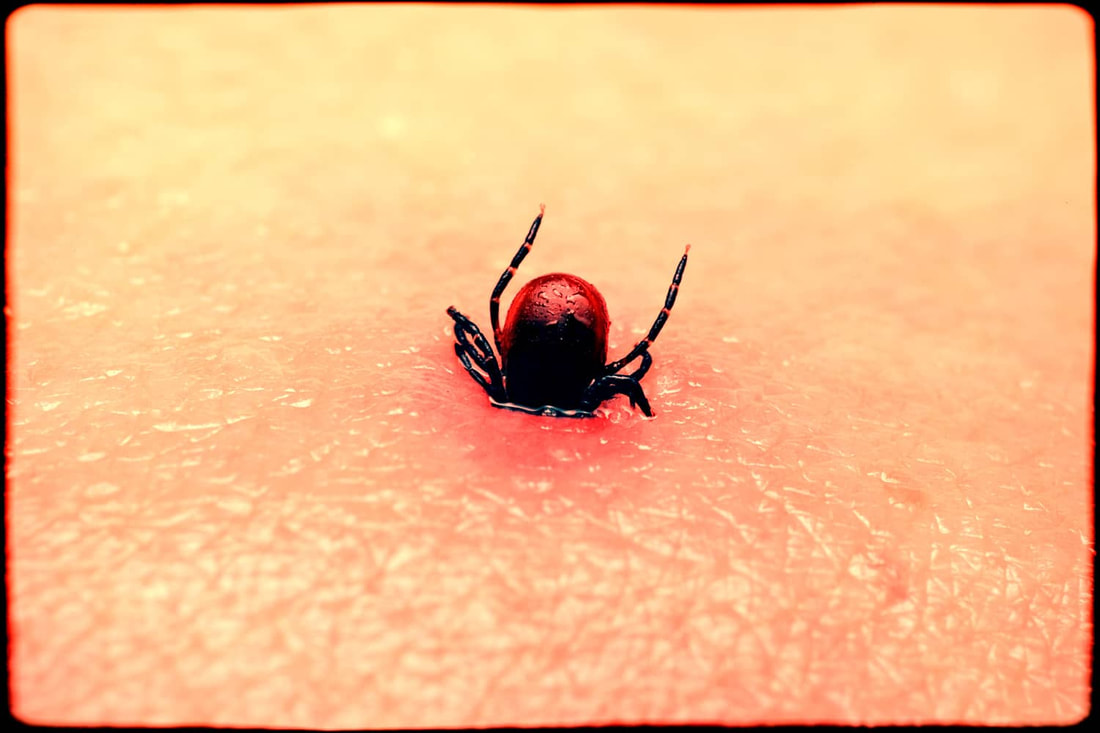
If you’ve ever been bitten by a tick you may have subsequently experienced symptoms of a rash, headache and fever that typically can last for up to four weeks. However, for some patients, tick-borne illness can have far-ranging and longer-term health implications stemming from the associated infection such as Bartonella, Ehrlichia, Babesia, or Anaplasma.
While you may not necessarily be familiar with the disorder “small fiber neuropathy (SFN)” it actually has a global prevalence of approximately four million individuals although the incidence is probably much higher than currently identified as quite often patients may not be fully evaluated for this condition.
Neurological effects post-COVID and what history tells us about post-viral syndromes. Results from a large retrospective study of nearly 240,000 subjects recently published in The Lancet show that in the six months after becoming ill with COVID, approximately one-third of the surviving patients were diagnosed with at least one neurological or psychological condition.1
New study identifies low sun exposure as risk factor in pediatric-onset MS. Lifestyles that keep us sofa-bound watching television, playing video games or sitting at a desk all day have definitely contributed to being labeled as the “indoor generation.”
As if the past year of ongoing challenges wasn’t enough, many of us have had to deal with the additional onslaught of even more trauma imposed by the recent winter storms. It really has been such a rough time for so many and we are concerned that these events can wreak havoc with our health, including our brain health, if left unchecked.
|
AuthorDr. Suzanne Gazda, Integrative Neurology Archives
February 2024
Categories |

















 RSS Feed
RSS Feed