|
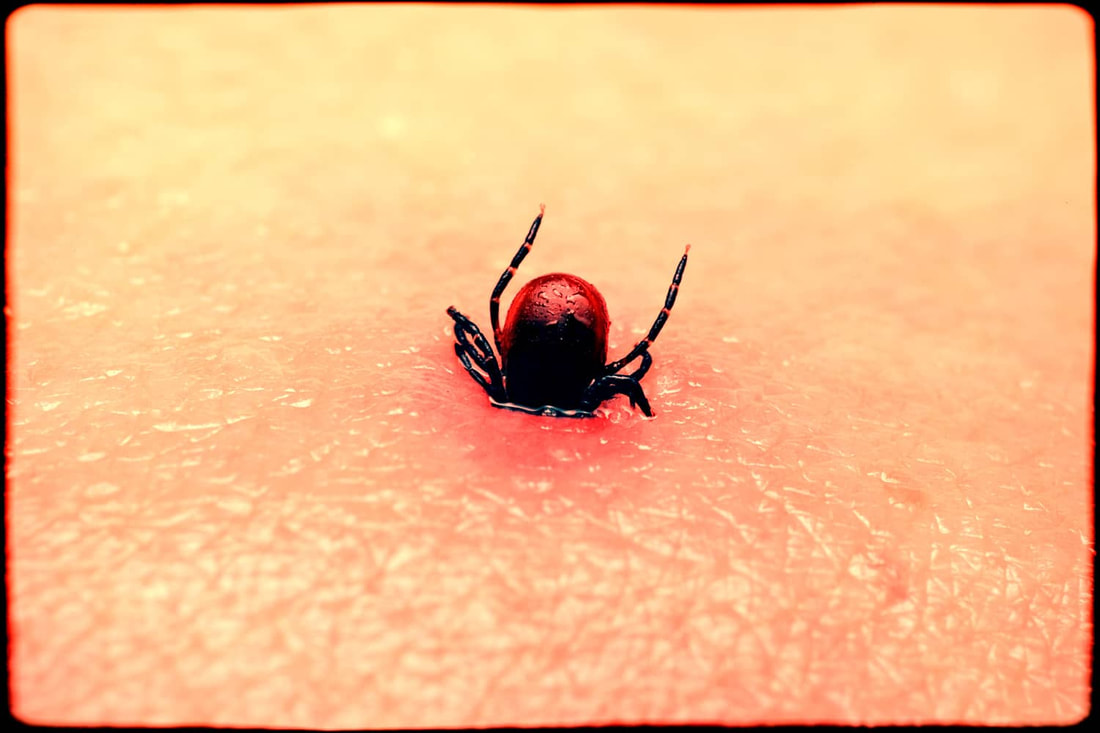
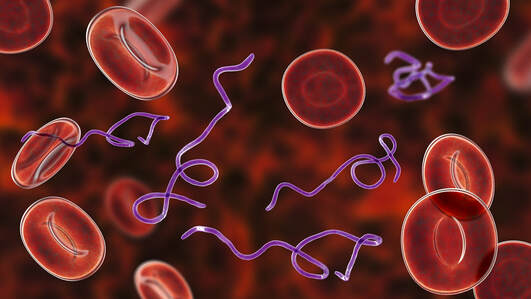
If you’ve ever been bitten by a tick you may have subsequently experienced symptoms of a rash, headache and fever that typically can last for up to four weeks. However, for some patients, tick-borne illness can have far-ranging and longer-term health implications stemming from the associated infection such as Bartonella, Ehrlichia, Babesia, or Anaplasma. Studies now find too that multi-systemic complications can also include neuropsychiatric issues, which along with numerous other challenges may be persistent and extremely debilitating. One published case study report involving a seven-year-old girl provided insight into not only Lyme disease, but also critical information about the infectious aspect linked to many neuroimmune disorders including pediatric acute-onset neuropsychiatric syndrome (PANS) and pediatric autoimmune neuropsychiatric disorders associated with streptococcus. This case report describes the diagnosis and treatment of the young patient with serological evidence of Lyme disease accompanied by multiple neuropsychiatric symptoms that began six months after visiting a tick endemic area of the U.S.1 Prior to the diagnosis of Lyme disease, the patient also met the clinical diagnostic criteria for PANDAS (Pediatric Autoimmune Neuropsychiatric Disorder Associated with Strep), with serological evidence of three distinct episodes of streptococcal pharyngitis. All three episodes of strep occurred during the six-month interval between suspected Lyme disease exposure and the onset of multiple neuropsychiatric symptoms. Her sometimes-incapacitating symptoms followed a relapsing and remitting course that impacted her personal, family, social, and academic domains. But over a period of approximately 30 months of treatment with various antimicrobials and three courses of intravenous immunoglobulins (IVIg) she experienced complete remission and remains symptom free at the time of published report. This review documents an increasing body of evidence and recognition that Lyme borreliosis and tick borne co-infections can trigger neurological and psychiatric symptoms. Authors stated that Borrelia can “cause immune and metabolic effects that result in a gradually developing spectrum of neuropsychiatric symptoms usually presenting with significant comorbidity which may include developmental disorders, autism spectrum disorders, schizoaffective disorders, bipolar disorder, depression, anxiety disorders (panic disorder, social anxiety disorder, generalized anxiety disorder, posttraumatic stress disorder, and intrusive symptoms), eating disorder, decreased libido, sleep disorder, addiction, opioid addiction, cognitive impairments, dementia, seizure disorders, suicide, violence, anhedonia, depersonalization, dissociative episodes, and other impairments." The report concluded with the admonition that physicians should be aware of the possibility that tick-borne infections could underlie an anorexia diagnosis and this potential link warrants further study. And still more evidence… In another complex case study, a 17-year-old female patient with several reported tick attachments during her childhood was diagnosed with anorexia nervosa (AN), an eating disorder marked by food and calorie restriction, after presenting with a myriad of neuropsychiatric symptoms. Authors detailed a history that was consistent with systemic infections and she tested serologically positive to Borrelia burgdorferi, Babesia microti, and Mycoplasma pneumoniae; in addition, her clinical presentation was consistent with a Bartonella infection.  They noted too that neuroinflammation occurs in both acute and persistent infection with Lyme borreliosis. Persistent infection with B. burgdorferi can induce chronic autoimmune disease and that anti-neuronal antibodies are present in many patients with persistent symptoms following treatment for Lyme borreliosis. After treatment with oral and intravenous antimicrobials, the patient stopped food restriction and no longer had body image concerns.2 Infectious impacts can play a major role in the development of autoimmune and neuroimmune conditions. It’s also important to recognize that Lyme disease may not always manifest what are commonly thought to be a bullseye rash and other more obvious signs. When patients present with neuropsychiatric symptoms and may have had any exposure to environments where ticks are populous, it’s crucial to conduct appropriate lab work. However - a negative standard Western blot does not necessarily rule out a diagnosis of a tick-borne illness; clinicians may want to consider repeat testing through a laboratory such as iGeneX that can conduct highly specialized assessments for Lyme-related pathogens. With any of these illnesses, especially when we are dealing with pediatric cases, we can’t let any stone go unturned in the search for not just a diagnosis, but also for a resolution for these patients. Nor can we undermine the potential for IVIG in helping overcome the challenges and abate the severity of symptoms. And in order to resolve “brain on fire,” all factors fueling the fire need to be addressed and treated! In hope and healing, Dr. Suzanne Gazda Questions or comments? Don’t hesitate to reach out to our offices. And if you are located in Texas or Colorado, let us know if we can provide more information about becoming a patient. References: 1 Cross A, Bouboulis D, Shimasaki C and Jones CR (2021) Case Report: PANDAS and Persistent Lyme Disease With Neuropsychiatric Symptoms: Treatment, Resolution, and Recovery. Front. Psychiatry 12:505941. doi: 10.3389/fpsyt.2021.505941 2 Kinderlehrer DA. Anorexia Nervosa Caused by Polymicrobial Tick-Borne Infections: A Case Study. Int Med Case Rep J. 2021;14:279-287 https://doi.org/10.2147/IMCRJ.S311516
0 Comments
Your comment will be posted after it is approved.
Leave a Reply. |
AuthorDr. Suzanne Gazda, Integrative Neurology Archives
February 2024
Categories |
 RSS Feed
RSS Feed