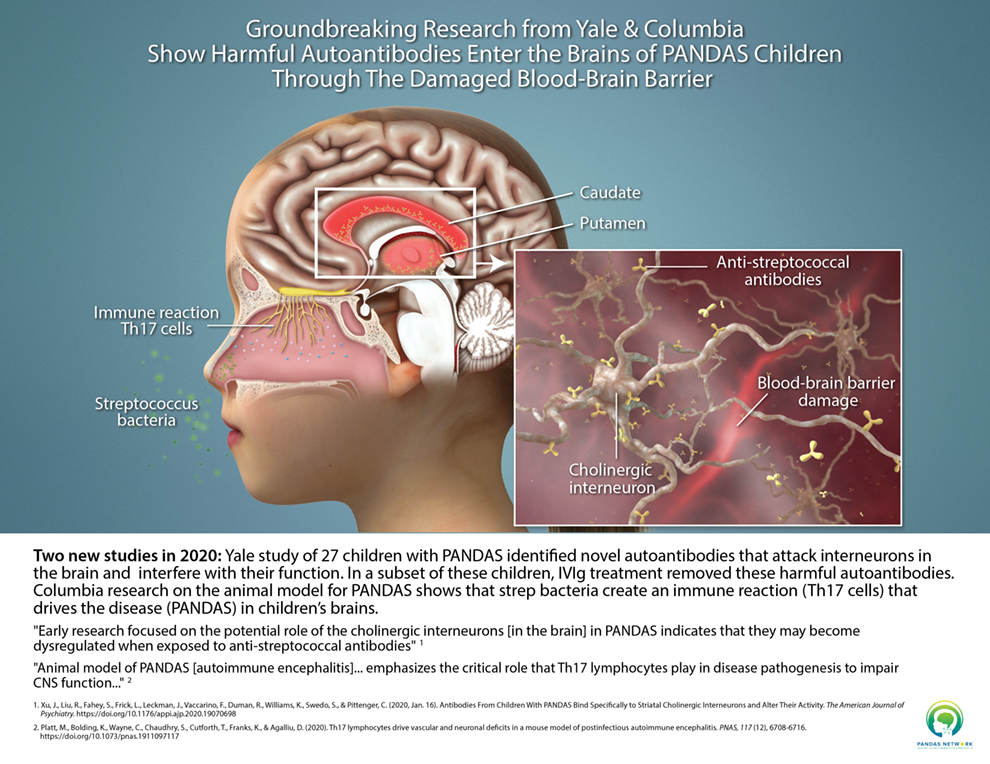
And this adds even more merit to our understanding of pathophysiological mechanisms involved in PANS (pediatric acute-onset neuropsychiatric syndrome) and PANDAS (pediatric autoimmune neurological disorder associated with streptococcal infection. While the effects of the global pandemic have been overwhelming, as one article notes, “amidst worldwide devastation including the loss of loved ones, financial turmoil, isolation, and tremendous stress, COVID-19 has provided the PANS community with something that years of pleading with the medical community failed to do.” Now, medical journals are replete with multiple studies that show the neurologic and psychiatric symptoms that may occur in the weeks and months after a COVID-19 infection. And even long after the infection clears, formerly healthy people are still experiencing severe related effects on mental health. Research spotlights interplay between the immune system, infection and effects on the brain. In a recent publication, immunologists from Yale School of Medicine and University of California San Francisco presented groundbreaking findings that show the misdirected autoimmune autoantibodies (proteins produced in response to a pathogen) that can mistakenly target and react with a person's own tissues or organs. This striking visual created by the PANDAS Network what occurred within the striatum area of the brains of the studied 27 children diagnosed with PANDAS. The striatum is part of the basal ganglia; in humans, it’s divided into the caudate and the putamen and has long been a target of research in obsessive compulsive disorder (OCD), Tourette’s syndrome, and PANDAS. Cholinergic interneurons (CINs) are one of several different types of interneurons in the striatum. They are critical regulators of brain activity and modify the signaling of other cells nearby. The striatum is involved in voluntary motor control; it has a role in cognition and reward processes, and it is involved in OCD. Researchers found that the autoantibodies discovered in PANDAS irritate and bind to CINS, but not to other neurons, providing “strong evidence for striatal CINs as a critical cellular target that may contribute to pathophysiology in children with rapid-onset OCD symptoms, and perhaps in other conditions.”1 Enter IVIG as potential treatment protocol. In the eleven children in the study who received intravenous immunoglobulin (IVIG) therapy, it diminished from the CINS. Symptoms of OCD and neuropsychiatric issues were calmed post-IVIG treatment. We know from prior research, infections triggers an immune response and subsequently cause the production of antibodies. In previous writing, we also noted the work of Dr. Dritan Agalliu and his findings that include:
With treatment, we can seek to remove both the source of infection AND the pathogenic antibodies. While degree of efficacy can be case dependent, when it works, treatment with IVIG may reduce or eliminate the antibodies that bind to the CINs, allowing them to function properly.  We know that PANS is triggered by infections other than strep and it is expected that there are overlapping mechanisms. We must remember how unlikely it is for each patient with these disorders to have exactly the same pathophysiological mechanisms, so it’s critical that individualized evaluations and treatment plans are implemented each and every time. For two decades, families whose children are stricken with symptoms of PANS and PANDAS have gone from one clinician or facility to another in search of help and answers that are often not forthcoming. Perhaps now, in the wake of a disease that has wreaked worldwide havoc but also highlighted the link between infection and brain health, we can at long last achieve more understanding and more relief for the many patients we strive to help every day. In hope and healing, Dr. Suzanne Gazda References: 1 Xu J, Liu RJ, Fahey S, et al. Antibodies From Children With PANDAS Bind Specifically to Striatal Cholinergic Interneurons and Alter Their Activity. Am J Psychiatry. 2021;178(1):48-64. doi:10.1176/appi.ajp.2020.19070698
0 Comments
Your comment will be posted after it is approved.
Leave a Reply. |
AuthorDr. Suzanne Gazda, Integrative Neurology Archives
February 2024
Categories |

 RSS Feed
RSS Feed