|
PART 8: The long COVID tsunami - what are the neurological implications?
What could be causing this puzzling war on the brain in the absence of viral infection? As we go through this blog series, we will explore why the Brain is being battered in Long COVID.
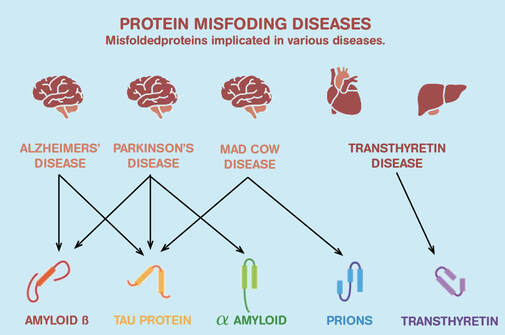
A compelling study published last year found the same genetic variants known to increase a person's risk of Alzheimer's were also associated with more severe forms of COVID-19. SARS-CoV-2 spike protein can form amyloid and toxic aggregates that can act as seeds to aggregate many of the misfolded brain proteins and can ultimately lead to neurodegeneration. In this study, findings showed how spike protein can induce protein misfolding with the outcome of toxic proteins like tau, alpha synuclein, prion, and amyloid. Note: We'd previously looked at whether there will be an increase in neurological disorders in our recent blog. And to get a better understanding about the role of amyloid, you can also watch: https://www.youtube.com/watch?v=7Ohzi-cU_J8&t=11s
Normal, healthy proteins will not aggregate to form amyloid. Unfortunately, with millions upon millions of copies of a given protein being made during our lifetimes, the folding process doesn't always occur correctly. When a protein misfolds and assumes the wrong shape, it may not properly fulfil its function, and may even become harmful. To minimize this occurrence, our cells have evolved a complex quality control system to correct or remove misfolded proteins. However, these systems become less effective as we age, allowing more and more errors to slip through the net. Once-healthy proteins can also misfold or partially unfold at some time after they have been made and released from a cell.
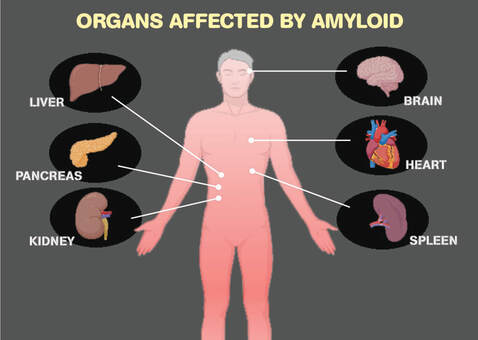
To date, 37 human amyloid proteins have been confirmed to be capable of causing disease. Well-known examples include amyloid β in Alzheimer's disease, α-synuclein in Parkinson's disease, and huntington in Huntington's disease. We also know that amyloid can contribute to diabetes and heart problems.
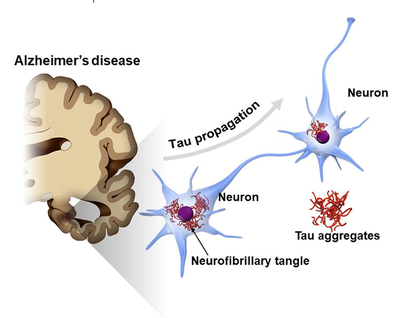
Amyloid formed from the breakdown of a larger protein, called amyloid precursor protein. One form, beta-amyloid 42, is thought to be especially toxic. In the Alzheimer's brain, abnormal levels of this naturally occurring protein clump together to form plaques that collect between neurons and disrupt cell functions.
Another excellent video to watch re: how Alzheimer's changes the brain: https://www.youtube.com/watch?v=0GXv3mHs9AU&t=52s
Spike Protein Inducing Amyloid Formation
In the recent study, "Amyloidogenesis of SARS COV 2 Spike Protein," researchers sought to examine if the spike protein in SARS-CoV-2 could be converted to amyloids in the body.
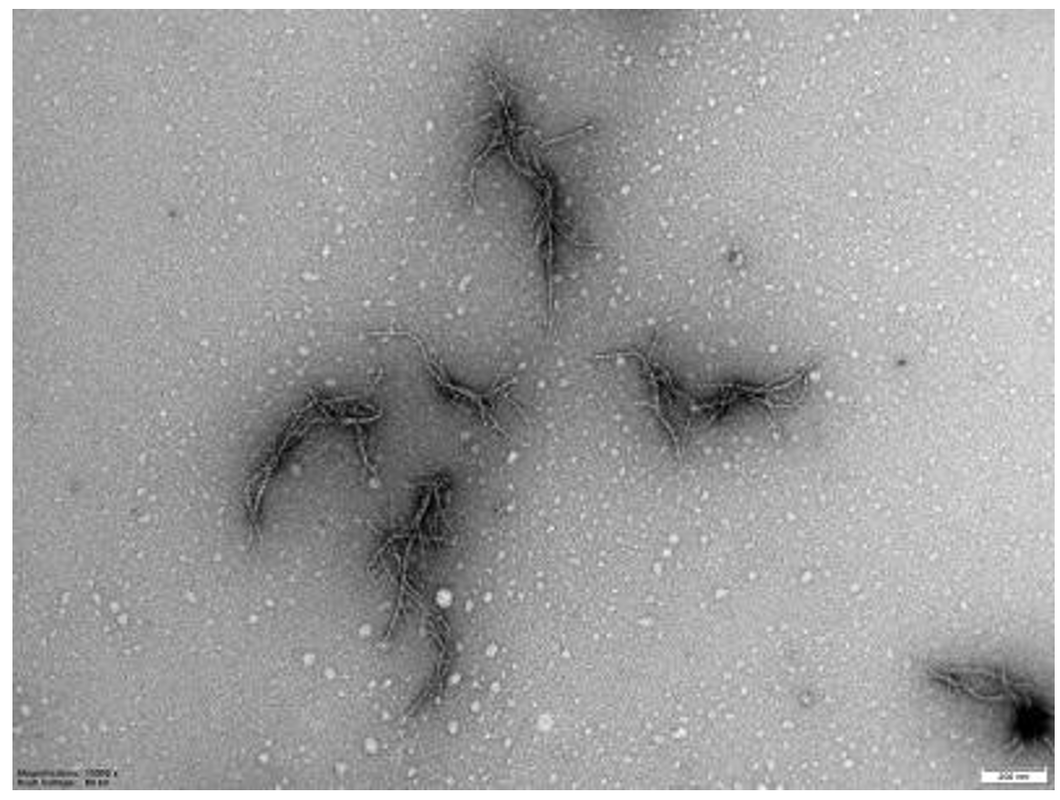
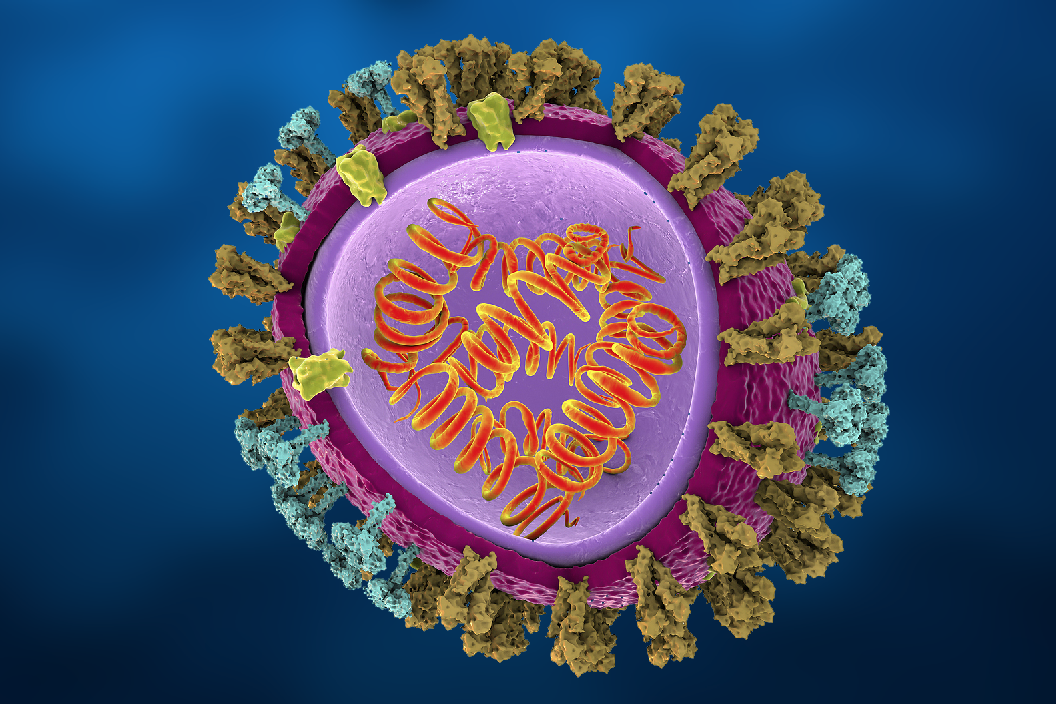
Picture of amyloid from the SARS-CoV-2 virus' spike protein, seen using an electron microscope. When the spike protein is mixed with the enzyme neutrophil elastase in test tubes, branched protein fibrils of amyloid are created, which potentially can cause disturbed blood coagulation in patients with COVID-19. This discovery shows a possible connection between harmful amyloid production and symptoms of COVID and Long Covid. Credit: Sofie Nystrom and Per Hammarstrom
The researchers said this after review of their data "We have never seen such perfect, but scary, fibrils as these ones from the amyloid-producing SARS-CoV-2 spike protein and pieces thereof."
This groundbreaking study reveals similarities between the effects of COVID-19 and the early stages of neurodegenerative disease such as Alzheimer's and Parkinson's. The researchers noted that there are many similarities between COVID-19-related symptoms and those which are observed in illnesses caused by misfolded proteins. And we know that a key molecular pathway implicated in diverse neurodegenerative diseases is the misfolding, aggregation, and accumulation of proteins in the brain.
Researchers led by Ina Vorberg, of the German Center for Neurodegenerative Diseases in Bonn, reported that two viral glycoproteins—VSV-G and the SARS-CoV2 S1 spike—dramatically boost the transfer of prions and misfolded tau between cells in culture and propose that SARS-CoV-2 spike S1 protein could facilitate the spreading of aggregated tau via the secretion of extracellular vesicles (EV) or direct cell-to-cell contact.
EVs like exosomes play a critical role in physiological processes, including synaptic transmission and nerve regeneration, but may also promote pathology in neurodegenerative disease as detailed in these studies: https://pubmed.ncbi.nlm.nih.gov/31312118/ https://www.frontiersin.org/articles/10.3389/fnins.2019.00698/full We have learned that spike protein is carried in exosomes for up to 4 months through the work of this study. Spike protein has prion-like domains.
In this study, "Prion-like Domains in Spike Protein of SARS-CoV-2 Differ across Its Variants and Enable Changes in Affinity to ACE2," the findings indicate that the identified prion domains in the SARS-CoV-2 receptor-binding domain (RBD) and ACE2 region that interact with RBD play important functional roles in viral adhesion and entry.
The question we are all asking is, in addition to the rise of neurodegenerative disease, will we see a rise of prion disease? There are 59 reports of CJD and prion diseases in VAERS to date (June 10, 2022). CJD has also been called ‘mad cow disease'. A quite rare, but very fatal neurodegenerative disease called Creutzfeldt-Jakob disease (CJD) leads to death within a year of diagnosis. According to the U.S. Centers for Disease Control and Prevention (CDC), this condition is triggered by the presence of the prion protein, a folded cellular glycoprotein that transmit its misfolded shape onto other normal variants of the same protein. The incidence of CJD in the US is 1/ million worldwide and about 350 cases per year in the US. Results from the Classen paper on covid vaccines and risk of prion disease indicate that the vaccine RNA has specific sequences that may induce TDP-43 and FUS to fold into their pathologic prion confirmations. The folding of TDP-43 and FUS into their pathologic prion confirmations is known to cause ALS, front temporal lobar degeneration, Alzheimer's disease, and other neurological degenerative diseases. A preprint French study suggests that the Pfizer, Moderna, and AstraZeneca vaccines may have contributed to the emergence of a new type of sporadic CJD that is much more aggressive and rapid in progression than the traditional form of the disease. This paper entitled "Towards the emergence of a new form of the neurodegenerative Creutzfeldt-Jakob disease: Twenty-six cases of CJD declared a few days after a COVID-19 vaccine” by the infamous Dr Luc Montagnier and his French colleagues, highlighted the presence of a Prion region in the different Spike proteins of the original SARS-CoV2 virus as well as of all its successive variants but also of all the vaccines (note the Prion region disappears completely in the Omicron variant). They reviewed 26 cases of CJD with first symptoms of CJD appeared on average 11.38 days after the injection of the COVID-19 vaccine. Of these 26 cases, 20 had died at the time of writing this article while 6 were still alive. The 20 deaths occurred only 4.76 months after the injection. Among them, 8 of them lead to a sudden death (2.5 months). They describe a "radically different and more aggressive form of CJD." Increased oxidative stress, alteration of key ion pathways and hyperadrenergic stress.
A study from researchers at Columbia University Vagelos College of Physicians and Surgeons reports that the brains of a small sample of patients who died of COVID display some of the same molecular changes found in the brains of people with Alzheimer’s disease.
The study published earlier this year looked at brain tissue from several deceased COVID-19 patients and found distinct parallels in brain damage with Alzheimer's patients. A significant body of recent research suggests that calcium ions “leaking” from certain ion channels in the brain, known as ryanodine receptors (RyR channels), may cause tau irregularities. Intracellular Ca2+ dysregulation is an underlying component of Alzheimer’s disease (AD) pathophysiology, and recent evidence implicates the ryanodine receptor (RyR) in the disease pathway.
Researchers found high levels of adrenergic and oxidative stress and activation of the TGF-β signaling pathway in the brain. RyR channels may be oxidized due to the activation of the TGF-β signaling pathway and the resultant remodeling of these channels could lead to neuropathology. This RyR2 remodeling results in intracellular Ca2+ leak, which can play a role in heart failure progression, pulmonary insufficiency, as well as cognitive dysfunction.
Many factors increase oxidative stress one of them being spike protein. Down regulation of ACE 2=increased TGFbeta=increased amyloid and Tau This research examines the inverse relationship between ACE 2 and upregulation of inflammatory pathways including TGF beta. And, even more worrisome is that reduced ACE 2 activity has been associated with tau hyperphosphorylation and increased amyloid in animal models. Spike protein interacts with and downregulates the ACE 2 receptors, as revealed in these journal publications: https://www.nature.com/articles/s41580-021-00418-x and downregulates ACE 2 https://www.ahajournals.org/doi/full/10.1161/CIRCRESAHA.121.318902 Learn more about the mechanism of tau and its neurological implications at: https://www.suzannegazdamd.com/scientifically-speaking1/alpha-synuclein-in-neurodegenerative-disease Learn more about ryanodine receptors and calcium leak leading to Alzheimer’s disease: https://www.researchgate.net/publication/317779778_Post-translational_remodeling_of_ryanodine_receptor_induces_calcium_leak_leading_to_Alzheimer's_disease-like_pathologies_and_cognitive_deficit
7 Comments
Peggy Phyna
11/2/2022 09:44:45 pm
Make me a promise Phyna, my mother said. "Promise me you won't put me in a home or make me live with one of your sisters". It was a joke at the time when my mom was just starting to forget things. 07/10/2020 was the hardest day of my life. Watching my mom talk to herself, packing her things 4-5 times a day, saying she has to go home. It was heartbreaking. I broke down and cried with her a few times and then I realized how hard it must be on my dad too. He can't leave the house, he has to convince her that she lives in their house. I came to the decision to quit my job. My dad needs help. I live 6 hours away but instead of visiting my parents, I'll be visiting my husband. My mom has always been there for me and been my best friend so I want to be there for her. I keep telling myself that I can snap her out of it. I got her numerous medications including RISPERDAL(RISPERIDONE), HALDOL(HALOPPERIDOL) THORAZINE(CHLORPROMAZINE) and TETRABENAZINE(XENAZINE) and DEUTETRABENAZINE (AUSTEDO), instead of helping her, they almost destroyed her due to the side effects. As I was reading more about Huntington's Disease on the internet, I met with some comments of people testifying about Dr. Bharat and his BUJAA HERBAL SUPPLEMENTS that it works for Huntington's. I contacted the doctor immediately and explained my mother's condition to him, he assured me that my mom will be fine and her memory will come back to normal. I ordered his Herbal Supplements and it was delivered to me here in Canada by DHL courier company in less than a week with instructions on how to use them attached in the package. After 3 weeks of using these herbs, we began to see improvement, after 6 months my mom was better, and it's been 2 years now and my mom is completely free from this horrible disease called huntington's. In case your loved one is suffering from huntington's disease I will advise you to use BUJAA HERBAL SUPPLEMENTS it may also help you. You can contact Dr. Bharat via email; [email protected] or Whatsapp him on: +393509392854.
Reply
Peggy Phyna
11/2/2022 09:45:56 pm
Make me a promise Phyna, my mother said. "Promise me you won't put me in a home or make me live with one of your sisters". It was a joke at the time when my mom was just starting to forget things. 07/10/2020 was the hardest day of my life. Watching my mom talk to herself, packing her things 4-5 times a day, saying she has to go home. It was heartbreaking. I broke down and cried with her a few times and then I realized how hard it must be on my dad too. He can't leave the house, he has to convince her that she lives in their house. I came to the decision to quit my job. My dad needs help. I live 6 hours away but instead of visiting my parents, I'll be visiting my husband. My mom has always been there for me and been my best friend so I want to be there for her. I keep telling myself that I can snap her out of it. I got her numerous medications including RISPERDAL(RISPERIDONE), HALDOL(HALOPPERIDOL) THORAZINE(CHLORPROMAZINE) and TETRABENAZINE(XENAZINE) and DEUTETRABENAZINE (AUSTEDO), instead of helping her, they almost destroyed her due to the side effects. As I was reading more about Huntington's Disease on the internet, I met with some comments of people testifying about Dr. Bharat and his BUJAA HERBAL SUPPLEMENTS that it works for Huntington's. I contacted the doctor immediately and explained my mother's condition to him, he assured me that my mom will be fine and her memory will come back to normal. I ordered his Herbal Supplements and it was delivered to me here in Canada by DHL courier company in less than a week with instructions on how to use them attached in the package. After 3 weeks of using these herbs, we began to see improvement, after 6 months my mom was better, and it's been 2 years now and my mom is completely free from this horrible disease called huntington's. In case your loved one is suffering from huntington's disease I will advise you to use BUJAA HERBAL SUPPLEMENTS it may also help you. You can contact Dr. Bharat via email; [email protected] or Whatsapp him on: +393509392854.
Reply
kia Colian
11/16/2022 04:29:59 pm
My name is Kia Colian from Birmingham City. I want to appreciate Dr. Bharat and his Herbal supplement BUJAA which helped my mom to return back to normal from memory decline. My mom was diagnosed with Huntington's disease in 2015 and ever since then it has been from one hospital to another and from one medication to the other which was accumulated with horrible side effects, I was so confused that I had to take her to a care home in August 2018. I visit her every week to have a chat and conversation and to see if she will get better but at a stage, it got worse that she doesn't recognize me anymore asking me who I am and who my mother is, I was so confused that I had to take her out from the care home. I was desperate to find a cure to this disease which led me to a video on YouTube where Dr. Bharat's name was mentioned in the comment section his contact was also there and immediately I contacted him and explained my mom's condition to him. He promised me that my mom would get well with his supplements, at first I doubted him because my doctor here told me that the disease has no cure but considering what I was going through I ordered the medications which were delivered to me 5 days later by DHL courier service. He sent me the instructions on how to administer them to her, some with warm water and others with cold water. I did as he instructed and in just 2 months I start seeing great improvement in her communications Dr. Bharat instructed me to allow her to do what she loves doing so she can be happy, my mom loves music very well, I play her favorite songs and watch her tap her foot and nod her head, I was so happy to see my mom improve in her mental ability to retain and recall our previous conversation. Today I am glad to share this testimony to the world that my mom is completely healed from Huntington's disease with BUJAA herbal medicine. For those suffering from Huntington disease or have any love ones suffer this deadly disease should contact doctor bharat now via: [email protected] or message him directly on WhatsApp via: +393509392854
Reply
Peggy Phyna
1/4/2023 03:51:16 pm
Make me a promise Phyna, my mother said. "Promise me you won't put me in a home or make me live with one of your sisters". It was a joke at the time when my mom was just starting to forget things. 07/10/2020 was the hardest day of my life. Watching my mom talk to herself, packing her things 4-5 times a day, saying she has to go home. It was heartbreaking. I broke down and cried with her a few times and then I realized how hard it must be on my dad too. He can't leave the house, he has to convince her that she lives in their house. I came to the decision to quit my job. My dad needs help. I live 6 hours away but instead of visiting my parents, I'll be visiting my husband. My mom has always been there for me and been my best friend so I want to be there for her. I keep telling myself that I can snap her out of it. I got her numerous medications including RISPERDAL(RISPERIDONE), HALDOL(HALOPERIDOL), THORAZINE(CHLORPROMAZINE) and TETRABENAZINE(XENAZINE) and DEUTETRABENAZINE (AUSTEDO) instead of helping her, they almost destroyed her due to the side effects. As I was reading more about Huntington's Disease on the internet, I met with some comments of people testifying about Dr. Bharat and his BUJAA HERBAL SUPPLEMENTS that it works for Huntington's. I contacted the doctor immediately and explained my mother's condition to him, he assured me that my mom will be fine and her memory will come back to normal. I ordered his Herbal Supplements and it was delivered to me here in Canada by DHL courier company in less than a week with instructions on how to use them attached in the package. After 3 weeks of using these herbs, we began to see improvement, after 6 months my mom was better, and it's been 2 years now and my mom is completely free from this horrible disease called Huntington's. In case your loved one is suffering from Huntington's disease I will advise you to use BUJAA HERBAL SUPPLEMENTS it may also help you. You can visit https://herbalcureforhuntingtondisease.blogspot.com/2022/06/09-2018-hope-for-huntington-disease.html to know more about BUJAA HERBAL SUPPLEMENTS or WhatsApp him on: +393509392854.
Reply
Professor Prem raj Pushpakaran
1/8/2023 04:46:54 am
Professor Prem raj Pushpakaran writes -- 2023 marks the birth centenary year of Daniel Carleton Gajdusek!!!
Reply
Tommy Latonia
1/14/2023 05:05:22 pm
Read carefully, it's said that Huntington disease has no cure, yes with the western medication but not with herbal medicine, my daughter's situation made me to realize that with doctor Bharat herbal medicine it can be cured. In 2014 she experienced difficulty in concentrating, memory lapses and depression, at first I thought it was stressed from her place of work until I took her to hospital and the doctor made me to understand that it's juvenile Huntington disease because she is still in her late 20s, which she inherited from my late husband that died of the same disease, the doctor told me it has no cure, but gave her some medicine which I noticed that it has side effects, my daughter situation got worst each day that passes, she was the best at her place of work, now a shadow of her self because of this deadly disease, she speaks to herself often, she was really going insane, I do not want to lose my daughter the same way I lost her father, in 2018 I carried out research on internet and bumped into a comment of a lady that got cured of Huntington disease, without wasting time I contacted doctor Bharat whose name was mentioned in the comment, now is been 3 years my daughter is living her best life again, for those that have the disease or have any love ones suffering from Huntington's disease, should contact doctor Bharat now on his mail via: [email protected] or text him directly on WhatsApp via: +393509392854
Reply
Your comment will be posted after it is approved.
Leave a Reply. |
AuthorSuzanne Gazda M.D. Neurologist Archives
January 2024
Categories |



 RSS Feed
RSS Feed