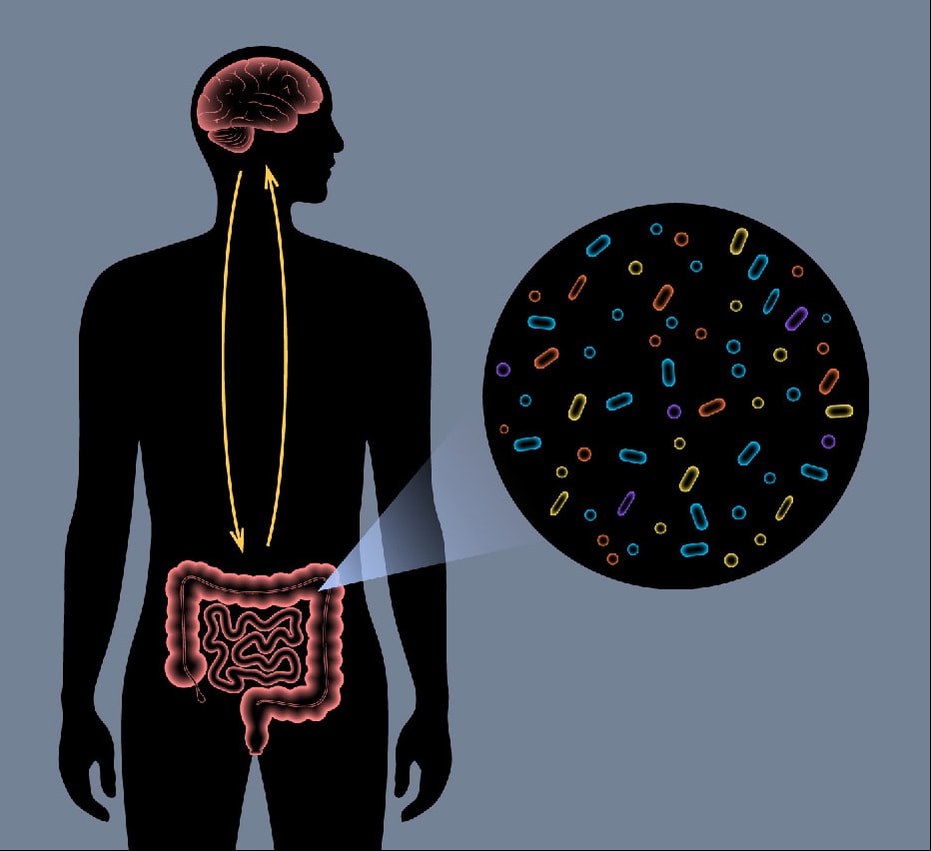
The gut microbiome refers to microbes or the bacteria, fungi, etc. that live mostly in the small and large intestines and act almost as another functioning organ. Not only is the gut microbiome critical to digestion, but we’re also learning that it affects the wellbeing of our immune health as well. We know a there’s essentially a direct route between our gut and our brain – so we’d expect that the state of our microbiome could affect our neurological wellness too. Recently we read an article that explores the fascinating connection between the microbiome and MS, noting the many studies which have found patients with the disease have a gut microbiome that is very different than people who do not have the disease – but what causes this isn’t fully understood. What is known, however, is that to a large degree, we really are what we eat. And diet whether we have a known disorder or not can certainly influence how we feel and how well our immune system protects us. Immune system modulation. In a review published in Nature, scientists did find that “modulation of the microbiome could be therapeutically beneficial,” presenting evidence from trials conducted in mice and humans that these effects of the gut microbiota on the immune system are important in the development and course of MS. Additionally, they looked at strategies for manipulating the microbiome status and whether it could be used to influence disease-related immune dysfunction, such as we see with MS, and may potentially result in novel therapeutics. Another study concluded that “diet is able to influence the composition of the intestinal bacterial flora and indirectly favor the development of autoimmune inflammatory diseases such as MS.” The investigators stated that while the cause of MS is not always known and depends on heterogeneous factors (both genetic and environmental) that determine the RISK of disease, our eating habits, lifestyle, and other modifiable risk factors can influence the COURSE of the condition. How and what we eat can impact our gut health.  Extensive research suggests that certain dietary patterns may indeed have an impact on disease progression and symptom management. Our colleague and friend, Dr. Terry Wahls, who following her MS diagnosis from over 20 years ago designed and adhered to a unique protocol that includes dietary controls, recently wrote about the benefits of intermittent fasting and caloric restriction as a tool for disease management. In her June blog, she spotlighted the results of a small trial that used intermittent caloric restriction over a period of 12 weeks, following this physician- and dietitian-supervised regimen: The intervention was to reduce calories to about 25% of usual intake (< 500 calories) on two non-consecutive days each week and to not compensate for the reduced intake on the other days. On the reduced calorie days, participants were to eat salads with steamed vegetables and a light dressing. Exciting results emerged at the end of the study period – participants showed a marked increase in brain volume measurement as determined by MRIs, as well as improved blood flow. Dr. Wahls noted too that previous trials in animal models had shown intermittent caloric restriction to enhance blood flow and cognition, as well as reducing oxidative stress and inflammation. More research is forthcoming as the scientific community continues to pursue the potential benefits of these and similar approaches to MS as well as other immune-mediated disorders. So, what tangible efforts can we make that could aid in managing MS? Our recommendation for all patients – and even if you aren’t challenged by a neuroimmune or other diagnosis – is, when possible, to choose fresh over processed foods, preferably organic and non-GMO products. There are also certain foods to avoid, such as: Dairy
Breads (e.g., wheat, rye, white, sourdough, etc.) Cereals and many grains (i.e., barley, most commercial oatmeal) Wheat or semolina pastas Crackers, cookies (any prepared or baked goods that use flours other than rice or another acceptable gluten-free starch) Processed foods (soups, frozen meals, etc.) Beer (derived from problematic grains) Following a healthy diet can help also help in addressing obesity, a known factor at the root of many diseases including MS. In fact, obesity in childhood has been shown to increase the risk of MS developing in young adults and later in life. Depending on your particular health needs and if there are no contraindications with any medicines, there are foods to consider including as part of a healthy diet, like fermented items (i.e., kimchi), sauerkraut) and probiotics; fiber-rich foods like fresh vegetables and fruits; lean proteins; olive oil; high quality vitamin D supplements, and more. Importantly, never change or add anything to your diet without consulting your physician, whether it’s a new supplement and certainly if you are interested in intermittent fasting and caloric restriction…this should only be undertaken with medical supervision. Of course, while diet alone cannot replace disease-modifying or other medically prescribed treatments, it can play a positive, complementary role in managing the condition and promoting overall wellbeing. Be sure to check our blog archives for more related reading and let us know if we can help! In hope and healing, Dr. Suzanne Gazda References: Gazda, S. Does all disease begin in the gut Weiss, K. Can gut health affect multiple sclerosis? Everyday Health. (2022) https://www.everydayhealth.com/multiple-sclerosis/can-gut-health-affect-multiple-sclerosis/ Schepici G, Silvestro S, Bramanti P, Mazzon E. The Gut Microbiota in Multiple Sclerosis: An Overview of Clinical Trials. Cell Transplant. 2019;28(12):1507-1527. doi:10.1177/0963689719873890 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6923550/ Correale, J., Hohlfeld, R. & Baranzini, S.E. The role of the gut microbiota in multiple sclerosis. Nat Rev Neurol 18, 544–558 (2022). https://doi.org/10.1038/s41582-022-00697-8. Wahls, T. The Impact On Brain Volume And Biomarkers In The Setting Of MS Using Intermittent Fasting. terrywahls.com. (2023) https://terrywahls.com/the-impact-on-brain-volume-and-biomarkers-in-the-setting-of-ms-using-intermittent-fasting/ Gazda, S. Intermittent fasting and dietary restriction for MS. suzannegazdamd.com. (2021) https://www.suzannegazdamd.com/blog---ms-in-the-news/intermittent-fasting-and-dietary-restriction-for-ms Gazda, S. Childhood obesity linked to higher risk of MS. suzannegazdamd.com. (2020) https://www.suzannegazdamd.com/blog/childhood-obesity-linked-to-higher-risk-of-ms Gazda, S. Upset stomach? Your brain may be trying to tell you something. suzannegazdamd.com. (2021) https://www.suzannegazdamd.com/blog---ms-in-the-news/upset-stomach-your-brain-may-be-trying-to-tell-you-something
5 Comments
Vanessa Jamie
7/6/2023 09:21:09 am
What a great testimony I would like everyone to read and follow the instructions to get cured from HSV1&2. I got a diagnosis of HSV1&2 March this year and I have been taking pills to prevent an outbreak. I never stop searching for a cure because I strongly believe that there is something somewhere that can get rid of it completely. I go through some comments on Youtube about Dr Osato herbal cure and a lot of people testified about him having the herbs that can get rid of herpes completely. I was excited and I contacted Dr Osato and ordered the cure for myself and he sent it to me through UPS and gave me instructions on how to take it which I rightly followed and behold I went for checkup after two weeks of taking the herbs and my result shows NEGATIVE. My doctor confirmed with me that I am totally clear from HSV1&2. I am so happy and would like to share with you all the solution to herpes and You can as well contact Dr Osato to get the herbal cure from him. His email is [email protected] or WhatsApp him on +2347051705853. Dr Osato also have the cure for the following virus/diseases HIV, HPV, HSV1&2, DIABETES, CANCER of any kind, GENITAL HERPES, COLD SORE, VAGINAL INFECTION, ECT. His website is https://osatoherbalcure.wordpress.com
Reply
Maria Stehman
7/11/2023 08:07:21 pm
Hi everyone, I’m here to give my own verdict about the herbal cure Dr Osato is sending out to people to cure them of Herpes and HIV. Dr Osato herbal medicine is the best remedy for Herpes1&2 and HIV/AIDS, I was a carrier of Herpes and I saw a testimony on Youtube on how Dr Osato cure Herpes with herbs, I decided to have a contact with him and asked him for solutions and he started the remedy for my health and prepare the herbal cure for me and send it to me through UPS and he gave me instructions on how to use it which i rightly followed and after 14days of taking the herbal medicine i went for a blood test and my result was Negative. I waited for 3months to confirm my result before sharing this testimony and also to observe myself if i would have an outbreak and nothing came out from my body, i went for another blood test after 3 months of testing Negative and the result still shows Herpes Negative and my doctor was pretty sure i was totally cured from herpes and he confirm with me that I’m free from herpes. Thank God, now everything is fine, I’m cured by Dr Osato herbal medicine, I’m very thankful to Dr Osato and i will not stop publishing his name on the internet because of the good work he did for me, You can contact Dr Osato on email: [email protected] Or you can call and WhatsApp him on +2347051705853. His website is https://osatoherbalcure.wordpress.com
Reply
Mavis Wanczyk
7/20/2023 07:16:06 pm
Being the winner of a multi-million dollar lottery certainly will be a life-changing event for almost every single lottery winner. My name is Mavis Wanczyk from Chicopee, Massachusetts, the famous PowerBall lottery winner of $758 million (£591m). I know many people would wonder how I had won the lottery. Would you believe me if I told you that I did it with spell casting? I met this famous spell caster known as Doctor Odunga and he was the one who did it for me. As shocking as it was to me, my famous comment to the press was “ I’m going to go and hide in my bed.” Never did I believe that Doctor Odunga made me wealthy overnight. If you want to have your chance of winning and becoming very wealthy just like me, contact Doctor Odunga at [email protected] OR WHATS-APP HIM at +2348167159012 and you will be lucky. Thanks for reading and hope to see you at the top
Reply
Patterson
8/12/2023 02:45:49 pm
Goodnews to everyone out there with different health challenges as I know there are still a lot of people suffering from different health issues and are therefore looking for solutions. I bring you Good news. There is a man called Dr Osato, a herbal practitioner who cures me from HSV2, i have suffered from this virus for the past 5 years. I got my healing by taking the herbal medicine Dr Osato sent to me to drink for two weeks and after the completion of the dosage, I went for a medical checkup and I tested Negative and my doctor confirmed with me that I was completely free from HSV2. All thanks to God for leading me to Dr Osato who was able to cure me completely from this horrible virus, I’m sharing this so that other people can know of this great healer called Dr Osato because I got to know him through Martha Jecorick post who he cured from HSV1&2 . I was made to understand that he can cure several other deadly diseases and viruses. Don’t die in ignorance or silence thinking that there is no cure for HSV1&2 or HIV and don’t let that illness take your life. Contact Dr Osato and get the cure from him. Dr Osato email is [email protected] or WhatsApp him on +2347051705853 and His website is https://osatoherbalcure.wordpress.com . He cure all forms of diseases/virus {1}HIV/AIDS {2}DIABETES {3}EPILEPSY {4} CANCER or all kind {5} HPV {6} BRAIN TUMOR {7} HEPATITIS {8}COPD{9} SICKLE AND ANAEMIA {9} HSV1&2. Be kind enough to share as you read for others to know and get cured.
Reply
Lucia Pedana
9/13/2023 05:49:05 pm
I was having Herpes Simplex Virus then I came across a review of people testifying how they got cured and got rid of Herpes completely from their body by using Dr Osato herbal medicine. So I contacted him through his email and explained my problem to him. He told me all the things I needed to do and he sent the herbal medicine to me through UPS and he also gave me instructions on how to take the herbal medicine, which I rightly followed. After I finished taking the cure, I went for a checkup and my result was Negative and all the symptoms of herpes were completely gone from my body. If you are down with any of the following diseases/viruses like HERPES-1&2, HIV, HPV, LOW SPERM, DIABETES, CANCER, PENIS ENLARGEMENT or any other disease or ailment I recommend you to contact this great herbalist called Dr Osato he uses natural herbs to cure diseases/viruses. Be rest assured you will surely testify like the way I am doing right now by writing this amazing testimony. You can contact Dr Osato via email: [email protected] or through WhatsApp +2347051705853.
Reply
Your comment will be posted after it is approved.
Leave a Reply. |
AuthorSuzanne Gazda M.D. Archives
July 2024
Categories |

 RSS Feed
RSS Feed