|
With numerous symptoms that challenge their lives every day, multiple sclerosis (MS) patients also appear to suffer almost twice as many migraine events as their healthy counterparts. According to a soon-to-be-published study, this represents nearly 24% of individuals with a MS diagnosis. First, some basic facts about migraine: it’s one of the most common chronic diseases in the United States and around the world, affecting roughly 15% and 14% of the populations respectively. Migraines are thought to be the result of interactions occurring between neurons, glial cells (which are the cells that help support, connect, and protect the neurons of the central and peripheral nervous systems), vasculature or the arrangement of blood vessels, and inflammatory signaling. Symptoms may include but are not limited to:
Read more about migraine in our previous blog at: https://www.suzannegazdamd.com/blog/migraines-the-science-causes-and-treatment-options MS is a neurological autoimmune disorder that has over the last 30 years become increasingly prevalent worldwide, which may be due in part to more sophisticated diagnostic tools, socioeconomic factors, and geographic influences. We have written extensively about the disorder, its potential treatments, and much more at https://www.suzannegazdamd.com/blog---ms-in-the-news. The National Multiple Sclerosis Society explains “Multiple sclerosis is a disease that impacts the brain, the spinal cord, and optic nerves, which make up the central nervous system and controls everything we do. The exact cause of MS is unknown, but we do know that something triggers the immune system to attack the CNS. The resulting damage to myelin, the protective layer insulating wire-like nerve fibers, disrupts signals to and from the brain. This interruption of communication signals causes unpredictable symptoms such as numbness, tingling, mood changes, memory problems, pain, fatigue, blindness and/or paralysis. Everyone’s experience with MS is different and these losses may be temporary or long lasting.” More evidence regarding a link. MS patients have a much higher risk of experiencing migraine symptoms than the general population. Additionally, migraine and MS patients share similar demographics, with the highest incidence among young, female patients with no history of another established condition. Many decades ago, studies began reporting on the MS/migraine connection. In 1952, Compston described a possible association, noting that 2% of patients develop migraine within three months of the onset of MS. The strongest evidence to date for an association between migraine and MS comes from a cohort study within the Nurses’ Health Study II. A 2012 study found that women with migraines prior to their diagnosis of MS had a 39% higher risk of developing MS when compared to the participants without migraines. What are the pathophysiological mechanisms between migraine and MS and MS and migraine? Some of the mechanisms contributing to the link between the disorders:
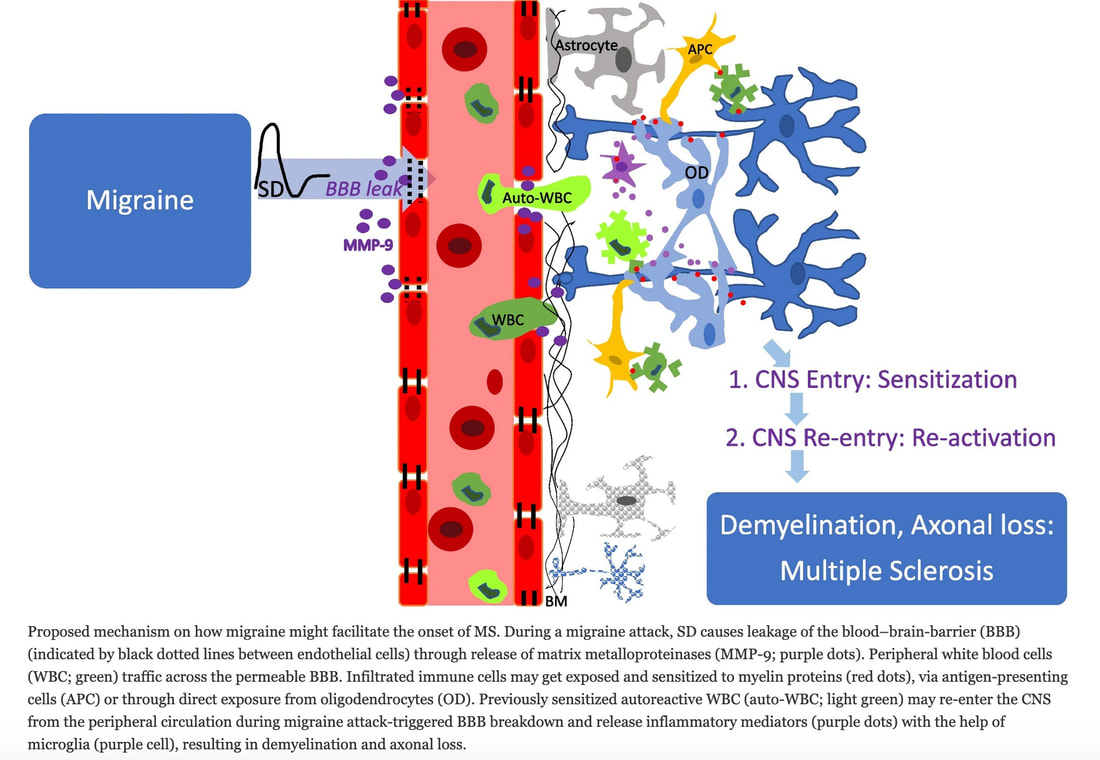
CSD, a slowly propagated wave of depolarization followed by suppression of brain activity, is a remarkably complex event that involves dramatic changes in neural and vascular function. This electrophysiologic event underlying migraine and an attack trigger may be a crucial factor for promoting MS onset by facilitating contact between peripheral immune cells and the usually privileged CNS structures. CSD may increase factors that influence the integrity of the blood–brain barrier permeability, thereby initiating neuroinflammation. Image credit: Huang, S.Y., Salomon, M. & Eikermann-Haerter, K. Advanced brain MRI may help understand the link between migraine and multiple sclerosis. J Headache Pain 24, 113 (2023). https://doi.org/10.1186/s10194-023-01645-7 In summary…
There are many environmental factors that may lead to the onset of migraine and multiple sclerosis – clearly, more research is needed to better understand the corresponding links between these disorders. As we have continually stressed in previous writings and in our clinical practice, lifestyle modifications also can be helpful not only in promoting general health and wellness, but in patients living with nearly any chronic disease. That’s why we also continue to encourage patients to be informed about your or your loved ones’ conditions and to be aware of all available resources! The American Migraine Foundation has a wealth of helpful literature regarding the disorder and potentially helpful lifestyle approaches to consider: https://americanmigrainefoundation.org/resource-library/lifestyle-changes-for-migraine/ And please visit our blog library as well for other related reading, including: https://www.suzannegazdamd.com/blog/study-shows-that-dietary-intervention-could-aid-migraine-sufferers https://www.suzannegazdamd.com/blog/migraine-remedies-can-a-drug-for-ms-or-natural-treatments-help https://www.suzannegazdamd.com/blog/what-if-there-was-another-way-to-treat-neuropathic-pain If you have questions or need to schedule a visit, please reach out to our offices – we’re here to help! In hope and health, Dr. Suzanne Gazda References: Mohammadi, M. et al. The association between multiple sclerosis and migraine: A meta-analysis. Multiple Sclerosis and Related Disorders. Volume 79, 2023. https://doi.org/10.1016/j.msard.2023.104954. https://www.sciencedirect.com/science/article/abs/pii/S2211034823004558 Headache Classification Committee of the International Headache Society (IHS) The International Classification of Headache Disorders, 3rd edition. Cephalalgia. 2018;38(1):1-211. doi:10.1177/0333102417738202 Stovner, L.J., Hagen, K., Linde, M. et al. The global prevalence of headache: an update, with analysis of the influences of methodological factors on prevalence estimates. J Headache Pain 23, 34 (2022). https://doi.org/10.1186/s10194-022-01402-2
4 Comments
Rachelle Hollie
11/7/2023 04:11:56 pm
I want to thank Dr Osato for curing me from HSV-2 with his herbal medication. All the symptoms of herpes are completely gone from my body and it's been over 3yrs now since i got cured from herpes with Dr Osato herbal medicine and my result still shows Negative and my doctor confirmed with me that I am totally cleared from herpes. I just want to let you all know that Dr Osato herbs cures herpes completely from the body and you can contact him for the cure if you are suffering from HIV/AIDS, HERPES-1 & 2, HPV, DIABETES AND CANCER. You can contact Dr Osato on his email: [email protected] or WhatsApp him on +2347051705853 to get the herbal product and get rid of the virus away from your body. Dr Osato is real and a great herbalist who can help you from your illness. His website is https://osatoherbalcure.wordpress.com or you can message him on his facebook page: https://www.facebook.com/Dr-Osato-Herbal-Cure-106002928040920
Reply
Lewis
11/29/2023 05:15:49 pm
I want to thank Dr Osato for the help he has rendered to me by getting Rid of my Herpes with his herbal medicine. I got Diagnosed of the herpes virus and after the Usage of Dr Osato Herbal Medicine, I was cured from Herpes and the virus was completely gone from my body. The Symptoms of Herpes Virus are completely gone.. So anyone who is having the virus should contact Dr OSATO to give you the herbal medicine to cure yourself. Dr Osato also has the cure for different types of diseases like HERPES 1$2, HIV, DIABETES, CANCER, HPV etc.. You can contact Dr Osato on email: [email protected] or call and whatsapp him on +2347051705853. His website is https://osatoherbalcure.wordpress.com
Reply
Ruth Cholay
1/16/2024 04:43:40 am
I'm here to let everyone know that there is a cure for HERPES1&2. The doctors have succeeded in letting people living with Herpes know that there is no cure for Herpes and they have been enslaved to the antiviral and other supplementary Orthodox medicine just to help suppress the virus and not a cure. I got diagnose of herpes1&2 and i did not believe in my doctor that no cure for herpes rather i went into research online and I was introduce to Dr Osato a herbal healer by a blogger who also narrated Her story online on how she was cured of Herpes after using Dr Osato Herbal Medicine. I got the herbal medicine from Dr Osato and made use of it as I was instructed. I went to the clinic for a checkup after two weeks of using the herbal product. My result came out Negative and I was booked for another appointment after 30days to confirm my result and the test still showed Negative and I was given the green light that I am fully free from herpes. All thanks to God for using this Great herbalist to heal me. You can contact Dr Osato by email: [email protected] or WhatsApp +2347051705853. His website is https://osatoherbalcure.wordpress.com. I have promised to keep sharing my testimony, so people will know that there is a cure for herpes.
Reply
Deame Romero
2/19/2024 06:12:54 am
There is a permanent cure for HSV1&2 and Dr Osato herbal medicine is the perfect cure for herpes and i have used it and i was cured from HSV1&2.The cure works perfectly with no side effects. Please i urge you to contact Dr Osato now and get the cure from him through his email address: [email protected] . His website is osatoherbalcure.wordpress.com and he is capable of curing HIV/AIDS, HERPES, HPV, HSV1&2, COLD SORE, CANCER of all kinds,DIABETES and so many other infections. Your perfect healing towards humanity is incomparable keep up your good work Dr Osato. His natural herbs for herpes work perfectly.
Reply
Your comment will be posted after it is approved.
Leave a Reply. |
AuthorSuzanne Gazda M.D. Archives
July 2024
Categories |

 RSS Feed
RSS Feed